Has My Uterus Been Saved?
How Can a General Surgeon Perform a Gynecologic Operation?
Africa Cries Out Report — Issue 16, 2026
Wang Haibin
April 4, 2026
It was another long day. When we finished dressing the final surgical wound, the clock read 9:20 p.m. Two consecutive days of nonstop operations—13 hours each—seems to have become the norm for the Africa Cries Out surgical mission team.
Looking at the 28 uterine fibroids of various sizes piled on the instrument table, then at the patient whose vital signs were stable, we all felt the joy of success. Yet at the same time, a question surfaced in everyone’s mind:
Was this truly the most reasonable choice?
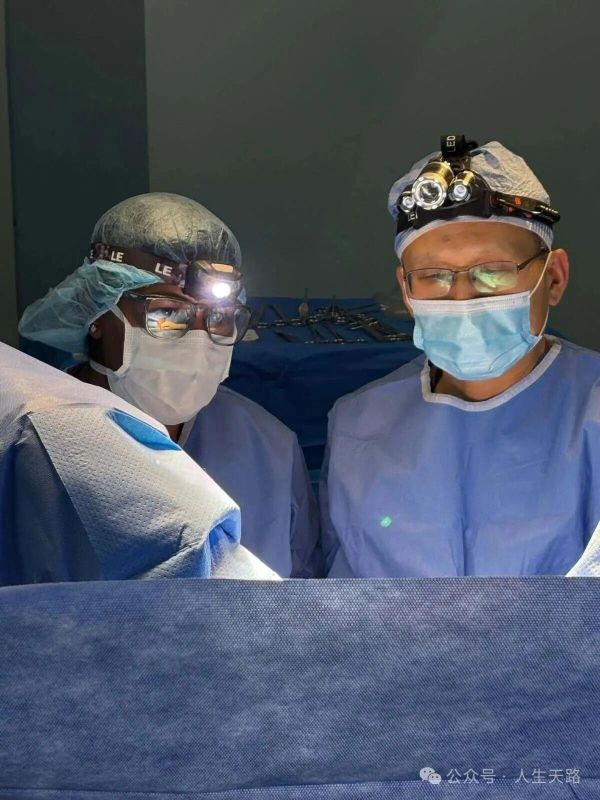
I clearly remember meeting this patient for the first time a few days earlier. According to the local hospital’s records, she was 36 years old, suffering from chronic bleeding caused by uterine fibroids, and infertile. She had undergone a previous myomectomy, but the fibroids had recurred. After an ultrasound, our gynecology team confirmed multiple fibroids. Considering she was still of childbearing age and strongly desired pregnancy, the team agreed to perform another myomectomy to preserve fertility. She then came to me for pre‑anesthesia evaluation.
However, when I reconfirmed her age, she became hesitant. Through the interpreter, she finally admitted that her actual age was 43—a full seven years older. Such discrepancies are common here due to the lack of a formal birth registration system; many children are registered years after birth with an approximate date.
But medically, 36 and 43 represent two completely different surgical pathways. At 43, fertility is already significantly reduced. With numerous fibroids, even after removal, her chances of conceiving would be extremely low. Clinically, the most reasonable option would be a total hysterectomy, which would fully resolve her pain and bleeding.
I had to report this new information to Dr. Jiang’s gynecology team. Through the interpreter, Dr. Jiang explained everything in detail and recommended a hysterectomy. But the patient firmly refused. She insisted on keeping her uterus, hoping she might still conceive.
On the day of surgery, Dr. Wu from our surgical team and Dr. Jacques, a local gynecologist, again explained the situation to the patient and her husband. They emphasized what would be the most medically appropriate choice. But the patient remained adamant: unless absolutely necessary, she would not accept a hysterectomy.
Out of respect for her wishes, we agreed to attempt a myomectomy, with the understanding that if life‑threatening complications arose, we might have no choice but to remove the uterus. Reluctantly, we proceeded with a plan that—strictly from a medical standpoint—was not the most reasonable.
Local pastor Felix M. revealed the deeper issue behind her insistence.
According to Muslim cultural norms, a woman’s security in the family depends heavily on her husband. Because she had been unable to conceive, her husband had long wanted to take a second wife. If he did, her status and livelihood would no longer be protected. Thus, removing her uterus would not only eliminate the possibility of pregnancy—it would fundamentally alter her position in the marriage.
In this context, fertility was not the true core issue.
Keeping the uterus—even with only a sliver of hope—was her way of preserving her rights and dignity within the family.
This is a surgical indication no medical textbook will ever teach. Here, the surgeon’s decision goes far beyond medicine; it must confront harsh social and ethical realities.
At this level, the “less reasonable” medical choice was, in fact, the best choice for the patient.
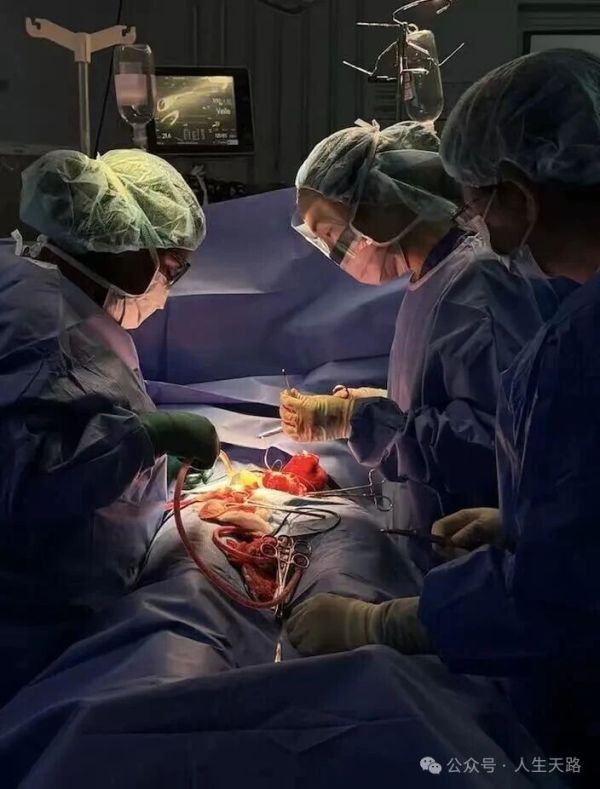
The team anticipated that this surgery would be extremely difficult and long. To ensure optimal conditions, Dr. Zhao, Dr. Cruz, and I decided to use a combined spinal‑epidural anesthesia technique.
As expected, once we opened the abdomen, we found the uterus covered with fibroids. Because of her previous surgery, extensive scar tissue had formed, causing severe adhesions between the posterior uterine wall and the small intestine. Separating these tissues was extremely challenging. To avoid injuring the bowel, the surgeons had to dissect very close to the uterine muscle, resulting in heavy bleeding.
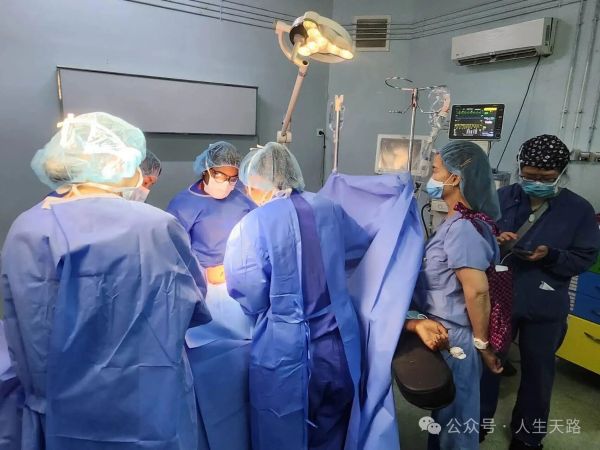
Dr. Zhang Niu—usually quiet and reserved, and today even “demoted” to serve as a temporary scrub nurse (though she is actually a highly experienced general surgeon)—took the tissue scissors from resident Dr. Raju and worked alongside Dr. Jiang to separate the adhesions. At times, the surgical field was completely submerged in blood. Yet the team did not panic, nor did anyone give up. The operation continued steadily through the blood.
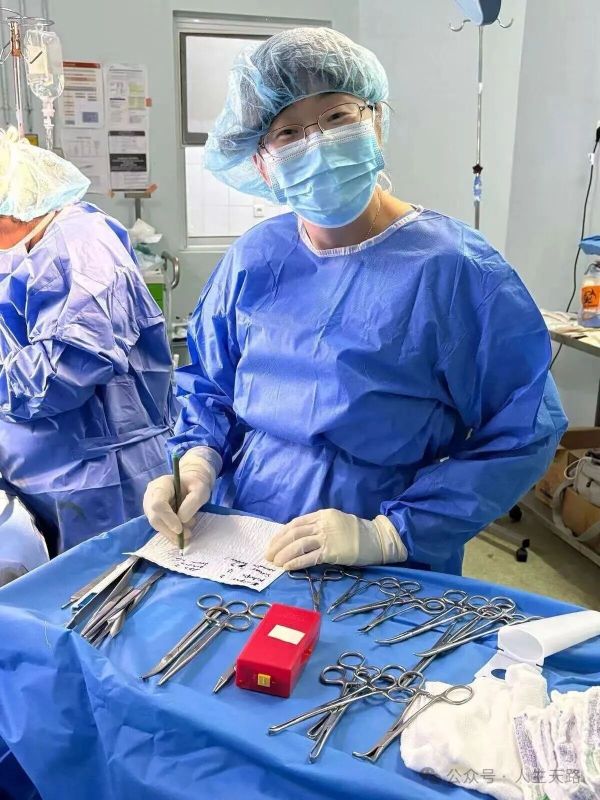
(Image: Dr. Zhang Niu assisting in surgery)
Due to massive blood loss, we had to transfuse the patient urgently. With no central blood bank in the local hospital, obtaining compatible blood is extremely difficult. Thankfully, our team had coordinated with local physicians in advance, ensuring a reliable supply.
The surgery lasted five and a half hours. When the spinal anesthesia began to wear off, we extended anesthesia through the epidural catheter and IV sedation to keep the patient comfortable. Ultimately, all 28 fibroids were successfully removed. Through the team’s seamless cooperation, we fulfilled the patient’s wish to preserve her uterus. When the final stitch closed her skin, we all breathed a deep sigh of relief.
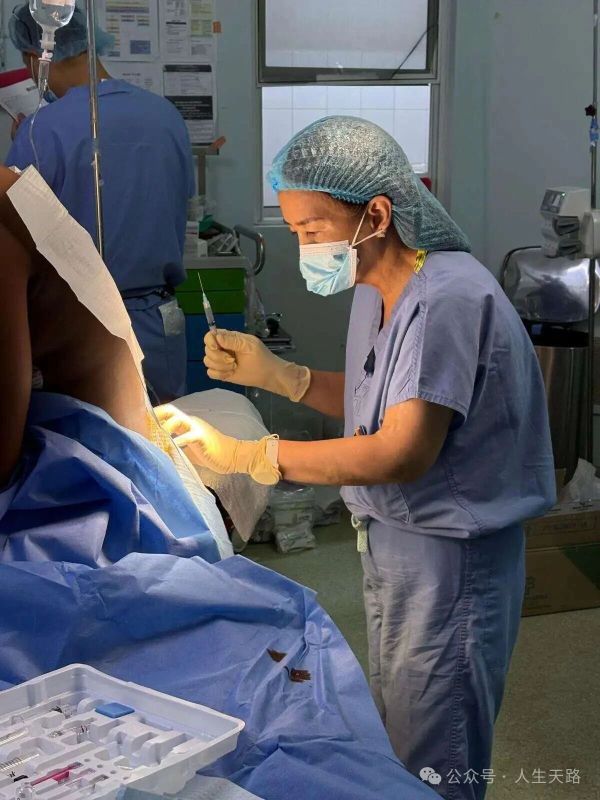
(Image: Dr. Cruz administering anesthesia)
Although we did not follow standard clinical guidelines, medicine is not only about technique—humanity and ethics are also essential. Patients live in the real world, each with unique circumstances shaped by family, marriage, culture, and religion. Understanding and respecting these realities—and choosing a treatment plan within reasonable limits rather than rigidly following textbooks—is itself a form of medical compassion.
I firmly believe that in the future, AI may replace doctors in diagnosis. But when it comes to empathy‑based humanistic care, machines will never be able to take our place.
At 10 p.m., the hospital was quiet. Exhausted, we looked at the patient sleeping peacefully under sedation. We hoped that our efforts would help preserve stability in her marriage and family. If so, then we had succeeded—because through our work, we preserved her hope.
And isn’t that the very purpose of medical missions—to bring hope?
Indeed, hope is the vitamin of life.

About the Author
Wang Haibin, MD, PhD
Anesthesiology & Pain Medicine Specialist
Based in Pittsburgh, Pennsylvania
Multiple‑time volunteer with Africa Cries Out
